By Deb Haines
How is rabies transmitted?
All species of mammals are susceptible to rabies virus infection, but only a few species are important as reservoirs for the disease. In the United States, distinct strains of rabies virus have been identified in raccoons, skunks, foxes, and coyotes. Several species of insectivorous bats are also reservoirs for strains of the rabies virus.
Transmission of rabies virus usually begins when infected saliva of a host is passed to an uninfected animal. The most common mode of rabies virus transmission is through the bite and virus-containing saliva of an infected host. Though transmission has been rarely documented via other routes such as contamination of mucous membranes (i.e., eyes, nose, mouth), aerosol transmission, and corneal and organ transplantations.
The Virus Travels through the Body
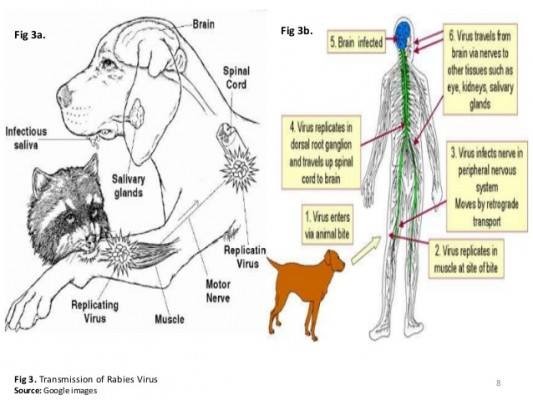
From numerous studies conducted on rabid dogs, cats, and ferrets, we know that when the rabies virus is introduced into a muscle through a bite from another animal, it travels from the site of the bite to the brain by moving within nerves. The animal does not appear ill during this time.
The time between the bite and the appearance of symptoms is called the incubation period and it may last for weeks to months. A bite by the animal during the incubation period does not carry a risk of rabies because the virus has not yet made it to the saliva.
The Virus Reaches the Brain
Late in the disease, after the virus has reached the brain and multiplied there to cause an inflammation of the brain, it moves from the brain to the salivary glands and saliva.
Also at this time, after the virus has multiplied in the brain, almost all animals begin to show the first sign of rabies. Most of these signs are obvious to even an untrained observer, but within a short period of time, usually within 3 to 5 days, the virus has caused enough damage to the brain that the animal begins to show unmistakable signs of rabies.
Extensive studies on dogs, cats, and ferrets show that the rabies virus can be excreted in the saliva of infected animals several days before illness is apparent. Such extensive studies have not been done for wildlife species, but it is known that wildlife species do excrete rabies virus in their saliva before the onset of signs of illness. The excretion of virus may be intermittent, and the relative amount of excreted virus may vary greatly over time, before and after the onset of clinical signs.
The reason there is so much variation in the time between exposure and the onset of the disease is that many factors come into play, including the site of the exposure, the type of rabies virus, and any immunity in the animal or person exposed.
What are the signs and symptoms of rabies?
The first symptoms of rabies may be very similar to those of the flu including general weakness or discomfort, fever, or headache. These symptoms may last for days.
There may be also discomfort or a prickling or itching sensation at the site of bite, progressing within days to symptoms of cerebral dysfunction, anxiety, confusion, agitation. As the disease progresses, the person may experience delirium, abnormal behavior, hallucinations, and insomnia.
The acute period of disease typically ends after 2 to 10 days. Once clinical signs of rabies appear, the disease is nearly always fatal, and treatment is typically supportive.
Disease prevention includes administration of both passive antibody, through an injection of human immune globulin and a round of injections with rabies vaccine.
Once a person begins to exhibit signs of the disease, survival is rare. To date less than 10 documented cases of human survival from clinical rabies have been reported and only two have not had a history of pre- or post exposure prophylaxis.


The Infectious path
- An animal is bitten by a rabid animal.
- Rabies virus from the infected saliva enters the wound.
- Rabies virus travels through the nerves to the spinal cord and brain. This process can last approximately 3 to 12 weeks. The animal has no signs of illness during this time.
- When it reaches the brain, the virus multiplies rapidly and passes to the salivary glands. The animal begins to show signs of the disease.
- The infected animal usually dies within 7 days of becoming sick.
What is the risk for my pet?
Any animal bitten or scratched by either a wild, carnivorous mammal or a bat that is not available for testing should be regarded as having been exposed to rabies.
Unvaccinated dogs, cats, and ferrets exposed to a rabid animal should be euthanized immediately. If the owner is unwilling to have this done, the animal should be placed in strict quarantine for 4 (dogs and cats) or 6 (ferrets) months. A rabies vaccine should be administered at the time of entry into quarantine. Every effort should be made to vaccinate the animal within 96 hours of exposure.
Animals with expired vaccinations need to be evaluated on a case-by-case basis. Dogs and cats that are currently vaccinated are kept under observation for 45 days.
Small mammals such as squirrels, rats, mice, hamsters, guinea pigs, gerbils, chipmunks, rabbits, and hares are almost never found to be infected with rabies and have not been known to cause rabies among humans in the United States. Bites by these animals are usually not considered a risk of rabies unless the animal was sick or behaving in any unusual manner and rabies is widespread in your area.
However, from 1985 through 1994, woodchucks accounted for 86% of the 368 cases of rabies among rodents reported to CDC. Woodchucks or groundhogs (Marmota monax) are the only rodents that may be frequently submitted to state health department because of a suspicion of rabies. In all cases involving rodents, the state or local health department should be consulted before a decision is made to initiate postexposure prophylaxis (PEP).
Is there rabies in my area?
Each state collects specific information about rabies, and is the best source for information on rabies in your area. In addition, the CDC publishes rabies surveillance data every year for the United States. The report, entitled Rabies Surveillance in the United States, contains information about the number of cases of rabies reported to CDC during the year, the animals reported rabid, maps showing where cases were reported for wild and domestic animals, and distribution maps showing outbreaks of rabies associated with specific animals.
How is rabies diagnosed?
In animals, rabies is diagnosed using the direct fluorescent antibody (DFA) test, which looks for the presence of rabies virus antigens in brain tissue. In humans, several tests are required.
Rapid and accurate laboratory diagnosis of rabies in humans and other animals is essential for timely administration of postexposure prophylaxis. Within a few hours, a diagnostic laboratory can determine whether or not an animal is rabid and inform the responsible medical personnel. The laboratory results may save a patient from unnecessary physical and psychological trauma, and financial burdens, if the animal is not rabid.
In addition, laboratory identification of positive rabies cases may aid in defining current epidemiologic patterns of disease and provide appropriate information for the development of rabies control programs.
The nature of rabies disease dictates that laboratory tests be standardized, rapid, sensitive, specific, economical, and reliable.
NOTE.….The incubation period for rabies can vary from two weeks to four months or even more. The speed at which clinical signs develop depends upon the site of the infection (the nearer the bite is to the brain and spinal cord, the quicker the virus reaches the nervous tissue), the severity of the bite, and the amount of virus injected by the bite.
Once the virus enters the body, it travels the nerves to the brain. Dogs and cats show a variety of signs, including fearfulness, aggression, excessive drooling, difficulty swallowing, staggering and seizures. In the first phase, the animal may undergo a marked change in temperament. A quiet animal may become agitated, while active pets become nervous or shy. Rabid wild animals may only display unusual behavior; for example, an animal that is usually only seen at night may be seen wandering in the daytime. In addition to those signs seen in dogs and cats, horses, cattle, sheep, and goats with rabies may exhibit depression, self mutilation, or increased sensitivity to light.
There are two recognized forms of the clinical disease: Furious rabies occurs when the rabid animal becomes highly excitable and displays evidence of a depraved appetite, eating and chewing stones, earth and rubbish (pica). Paralysis eventually sets in and the rabid animal may be unable to eat or drink. Hydrophobia (fear of water) is not a sign of rabies in dogs and cats. This is a feature of human rabies. The animal finally dies in a violent seizure. Dumb rabies is the common form. There is progressive paralysis involving the limbs, distortion of the face and a similar difficulty swallowing. Owners will frequently think the animal has something stuck in the mouth or throat. Care should be taken in examination since rabies may be transmitted by saliva. Ultimately the animal becomes comatose and dies.
(Information based on material written by Ernest E. Ward, Jr., DVM, and from the American Veterinary Medical Association)
Info provided from Center Of Disease Control ….https://www.cdc.gov/rabies/transmission/body.html
https://www.mebanepet.com/what-are-the-signs-of-rabies-part-v-of-rabies-101/
**The Vet Corner groups encourage members to establish a relationship with their local veterinarian, don’t wait until an emergency.**
© 2014-2025 Rural Veterinary Outreach. All Rights Reserved.

You must be logged in to post a comment.