By Dr. AJ Warren
Introduction
Osteoarthritis (O.A.) is one of the most common diseases in dogs, and until recently was often ignored or put down to ‘old age stiffness’. We now know that 80% of all dogs over the age of 8 have some level of OA, and 20% of dogs of all ages have it. Some breeds are more predisposed than others; for example Labradors (hips & elbows) and German Shepards (hips, spine & hind legs). Large breed and giant dogs ( e.g. Husky, Boxers, Great Danes ) are more likely to have it, and more likely to see it earlier than smaller dogs. Dogs that are very active during their youth ( e.g. working collies and spaniels ) or dogs that are chronically overweight are more likely to have it as well.
What is O.A.?
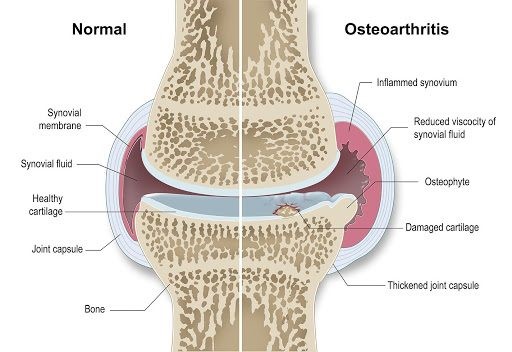
O.A. is a disabling, non-curable, and progressive disease which initially focuses on moving joints but eventually affects the whole dog and is a major cause of euthanasia due to loss of quality of life. The disease process begins with a degeneration of the cartilage within a joint. Cartilage has a poor blood supply and no nerve supply so this in itself isn’t known to be particularly painful, but it also unfortunately means that cartilage has very minimal regenerative healing properties. Once the protective cartilage has worn away, the underlying bone is exposed. Bone has a good nerve and blood supply so when the bone grinds against bone this causes a painful inflammatory response. The dog will compensate for this painful joint by reducing it’s level of movement, resulting in weakened muscles and more stress put on other joints in the body – this in turn can speed up the degeneration of cartilage in other joints.
How do I spot the signs? ( for more information visit : caninearthritis.co.uk/what-is-arthritis/identifying-signs )
Chronic pain can be debilitating, but sadly dogs have no way of telling us so they tend to just ‘get on with it’. Most dogs will not yelp or vocalise (unless there is an acute, trauma-related flare-up) or go off their food (as a predator species, the drive to eat is very intense!). Sometimes they will offer more subtle signs;
| – Panting – Lip licking – Licking at paws or joints – Stiffness in the mornings – Stopping to rest on walks | – Disliking slippery floors – Sleeping more – Seeming ‘skinny’ around the rear end due to muscle wastage – Reluctance to jump (e.g. into the car) |
Not all dogs will refuse to go on walks; they are their favourite part of the day and no amount of pain or discomfort will stop them from going out! These are the animals that may still willingly go for hours on end – despite the pain.
How Can I prevent O.A.?
O.A. can be put off through careful selection and management in younger dogs. Choose your puppy from a reputable breeder who has undertaken hip and elbow-scoring on the parents (in predisposed breeds) to limit the risk of genetic predisposition.
Do not over-exercise puppies, especially those with known predispositions. A good rule of thumb is ‘5 minutes a month’; if you have a 3 month old puppy, they should only have 15 minutes ( 3 x 5 ) of exercise at a time. Most puppies will regulate their own exercise well – they’ll run around and play for a few minutes and rest for a few hours. This is GOOD and will allow them to develop their muscles and joints properly.
Different breeds will reach skeletal maturity at different ages; smaller breeds may be mature at 8-12 months whereas larger breeds may not be mature until 18 months. Some dogs (e.g. working dogs) will need to do a lot of intensive exercise from day to day, but where possible try to wait until they are skeletally mature. A 6 month old Labrador shouldn’t be jogging 10 miles a day!
Avoid excessive ball-throwing! This can be a fun game to play but this is a high-impact exercise that puts a lot of pressure on joints as dogs twist, turn and jump at high speeds. These movements are particularly high risk for animals with open growth plates (skeletally immature).
Keep them lean! Some studies suggest up to 80% of British pets are overweight or obese and there is a known link between obesity and joint disease. A dog should have a body condition score of 4.5/9 ( 1 = emaciated, 9 = obese ) where you can feel the ribs easily and a waist is visible. Weigh your dog often and follow the chart on the back of their food packet. Avoid treats or table scraps and contact your vet for further advice if you’re struggling to get the weight off!
Visit Royal Canin – Body Condition Score for more information, and a useful chart.
Some brands offer a Joint & mobility food. These may be beneficial to some dogs, but work best when fed exclusively. Royal Canin, Hills and Purina are some of the better-known brands, but your vet will be able to advise on the suitability of other brands.
Supplements
Some supplements have shown to protecting effects, but you do have to be careful which ones you choose as most of the supplements available have little or no studies to support their use. Yu-Move, Yu-Move advance, Nutraquin +, Synoquin and Vetpro Joints and mobility are some of the supplements that have supportive studies. You want to choose products with the following ingredients
- Glucosamine Hydrochloride (HCl)
- Some products contain Glucosamine Sulphate instead, but Glucosamine HCl is much stronger and more concentrated, and is more beneficial in studies.
- Hyaluronic Acid
- Chondroitin
- Injectable Chondroitin has proven benefits but there is still debate over its efficacy when taken orally
- Omega-3 source ( e.g. Green-lipped mussel )
- Omega-3’s are anti-inflammatory but Omega-6’s are pro-inflammatory so make sure you get the right one!
- Boswellia extract
- It’s unknown how it works but studies suggest it may have pain-relieving properties
Be mindful when feeding oils (fish, coconut etc ) as though these contain Omega 3 (anti-inflammatory) they also contain Omega 6 (pro-inflammatory) and can be very high calorie which may make it harder to keep them lean. Be wary of products relying on Turmeric as the active ingredient; though curcumin (which is a partial component of turmeric) has some evidence to suggest anti-inflammatory properties, this was only observed in humans, and only when when curcumin was dosed in very high levels (much more than in a standard tub of turmeric ).
Remember that supplements are a good adjuvant therapy and can help prevent joint disease, but they are not a substitute for appropriate management. Similarly, they cannot be used in place of anti-inflammatory drugs once the disease process reaches a certain point.
How Can I Treat O.A?
Treatment falls into two main categories;
- (Owner-led) Management changes
- No jumping up/down (e.g into the car, off the sofa)
- Minimising stairs
- Avoiding slippery floors
- Less-is-more exercise ( little and often rather than sporadic long walks, focusing on sniffing and exploration rather than running and chasing )
Changing the dog’s management is THE singular most important thing you can do for your dog!
Visit the following pages for comprehensive advice about management changes
- Canine Arthritis Management – YOUR DOG, ARTHRITIS & HOW CAM CAN HELP WATCH HANNAH’S VIDEOS!
- Canine Arthritis Mangement – What TO AVOID
- (Veterinary-Led) Medical or Surgical Approaches
Surgical Approaches
Surgery is not always appropriate in older dogs; during recovery periods, dogs have to keep the weight off of the affected limb which can cause further degeneration in compensating limbs.
However in animals where one joint / limb is significantly more effected than the others (e.g. in a previously-injured knee) surgical intervention may offer a long-term solution. Sometimes surgeons will enter the joint, flush away the inflammatory processed and gently remove flaps of bone or cartilage that may be causing further damage (arthroscopy). Other times, they may offer a full replacement joint (e.g. a false hip).
These are often specialist surgeries and may need referral from your G.P. vet following a series of diagnostic x-rays to ensure the referral clinic knows exactly what surgery may be in the dog’s best interest.
For many older patients we may recommend a more conservative, medical approach.
Medical Approaches ( Always work best when combined with management changes!)
We will often use a range of complementary medications when treating O.A. We usually start with a method of reducing the inflammation, followed by additional pain relief when needed. It is possible to combine a whole host of different drugs; so long as they work in different ways within the body you can get a cumulative therapeutic effect whilst limiting risks and possible side effects.
- Non-Steroidal Anti-Inflammatories (NSAID’s)
- Often first line of treatment as this targets the inflammation and acts as a pain relief. There are many different types and while many work in similar ways, there is a variety to choose from. They cannot be combined with each other, but most can be combined with other therapies*. See the chart below.
* Except Steroids – these can not be combined with NSAID’s.
- Steroids (Prednisolone, Medrone-V)
- Rarely used these days for treatment of O.A.; potent anti-inflammatory but no pain-relieving properties and has risk of many side effects including weight gain.
- Cannot be given alongside NSAID’s
- Pentosan Polysulphate (Cartrophen, Osteopen)
- Series of 4 injections given a week apart. Sometimes a full course is given every 3 months, sometimes a ‘top up’ injection is given monthly – it’s case dependent.
- Works to help protect and strengthen the cartilage, and prevent further breakdown.
- May have some pain-relieving properties, secondary to anti-inflammatory effects
- An effect is seen in approx. 80% of dogs.
- Can be given in conjunction with NSAID’s* or steroids
- *Can’t dose with NSAID on same day as injection.
- Monoclonal Antibody (Librela)
- Series of 2 injections, 4 weeks apart, with ‘top up’ injections as needed.
- Works by targeting specific receptors associated with O.A. pain
- No anti-inflammatory properties; this is purely a pain-relief
- Can be given in conjunction with NSAID’s *
- In humans administration of this drug is contra-indicated alongside NSAID’s but the disease process is different and similar issues have not been reported in dogs.
- Co-Codamol (Pardale-V)
- Specially formulated for dogs (different formulation to the human equivalent)
- Purely pain relieving; no anti-inflammatory effects
- Can be given alongside NSAID’s*
- Some vets may recommend a lower dose if used long-term alongside NSAID’s.
- If combined with NSAID’s bloods may be warrented more often to check liver and kidney values
- Gabapentin
- Particularly good for dogs with concurrent nerve pain (e.g. spondylosis of the spine, degenerative myelopathy)
- May cause mild sedative effects (useful if you have a bouncy dog who needs to rest)
- Cannot be stopped suddenly – doses have to be increased or decreased gradually
- Can be given in conjunction with NSAID
- Fairly controlled drug – we have to be careful how much we give out
- Amantadine
- Reduces development of sensitisation to pain in the central nervous system (e.g. brain and spinal cord)
- Needs to be given in conjunction with NSAID
- Tramadol (Tralieve, Tramvetol)
- Previously thought to be as effective in dogs as it is in humans, tramadol used to be a favourite amongst veterinarians.Unfortunately more recent studies suggest it doesn’t control pain as well as previously thought, so it is rarely being used as a first or second-choice drug.
- May still have some pain relieving effects – more likely to have a dissociation effect (so the dog is less aware of the pain)
- Can be given alongside NSAID’s and steroids
- Possible mild sedative effect
- Tightly controlled drug – we cannot give out large amounts of this drug for safety reasons.
Common NSAID’s (Non-Steroidal Anti-Inflammatories)
| Drug | Pros | Cons |
| Meloxicam ( Metacam, Melododyl, Loxicom, Rheumacam, Inflacam ) | Tasty liquidEasy to dose accuratelyCheapGiven with food | Older product so can cause stomach upsetCan stress the kidneys (so routine bloodwork is advised for monitoring purposes) |
| Carprofen (Rimadyl) | Tasty tabletCheapOnce or twice daily dosing | Older product so can cause stomach upsetSlightly less accurate dosing (dosed within a range)Can stress the kidneys (so routine bloodwork is advised for monitoring purposes) |
| Robenacoxib (Onsior) | Newer product (more selective) so less likely to cause stomach upsetMay be more tolerable to dogs who react to MeloxicamGiven with or without foodDesigned specifically for O.A in dogs *There is some evidence to suggest Firocoxib may be slightly more effective than Onsior, particularly in acute flare-ups. | Slightly less accurate dosing (dosed within a range)Can stress the kidneys (so routine bloodwork is advised for monitoring purposes)Slightly more expensive than Meloxicam or Rimadyl |
| Cimicoxib ( Cimalgex ) | ||
| Firocoxib (Previcox) | ||
| Grapiprant (Galliprant) | New product. Works differently to traditional NSAID’s – it block pain without interfering with other homeostatic mechanisms.Likely to be more tolerable to dogs who react to MeloxicamGiven on empty stomach, 60 mins before food.Designed specifically for O.A in dogs | Slightly less accurate dosing (dosed within a range)Can stress the kidneys (so routine bloodwork is advised for monitoring purposes)Slightly more expensive |
Additional Therapies
There are a variety of alternative / adjuvant therapies available for helping to treat O.A. Some have more proven benefits than others, and it’s worth discussing with your vet which one may be beneficial to your pet. Remember that not all these job titles are protected (which means not everyone offering these services has the same qualification or training) so it’s always worth checking out the qualifications before engaging in services; Registered vets (MRCVS), Registered Vet Nurses (RVN) and Chartered Physiotherapists (ACPAT) are reliable, but your vet may be able to direct you to other individuals with different, but equivocal qualifications.
Hydrotherapy
- Aims to increase muscle mass and fitness whilst reducing fat, the water helps to reduce the loading on the joints whilst encouraging increased oxygen flow to tissues. Treadmill tanks are often considered more effective than swimming pools as they encourage more complete movement (pure swimming sometimes results in favouring the affected limb). Suitable for animals with muscle wastage, but who’s pain is well controlled.
Physiotherapy
- Aims to increase range of motion through massage and stretching, whilst minimising impact to the joints.
Laser
- Class 4 lasers have shown to have some effect in promoting healing, by increasing the levels of ATP (energy) within cells. The evidence is limited, but may be suitable for animals who’s pain is not controlled well enough for hydro or physiotherapy. Class 3 and below are often not powerful enough to do much.
Acupuncture / Acupressure
- When practiced correctly, there is emerging evidence to suggest is can stimulate the body’s repair mechanisms in the nervous system, immune system, and hormonal and cellular systems.
If you have any questions, ALWAYS contact your veterinarian!
Much of this advice is similar for cats but remember cats require different doses of drugs, and cannot tolerate certain drugs designed for dogs or humans. Always talk to your vet before giving a cat a medication prescribed for a dog.

Useful Resources
More about Arthritis – www.caninearthritis.co.uk
Find a physiotherapist – www.acpat.org/
Find a Hydrotherapist – www.canine-hydrotherapy.org/
More about Laser therapy (K-Laser) –
www.klaser.co.uk/KLaser-information-for-pet-owners.aspx?clientId=20180
Links to supplements
Yumove – yumove.co.uk
Synoquin – www.vetplusglobal.com/products/synoquin-efa/
Nutraquin + – www.nutravet.co.uk/nutraquin
Vetpro Joints – www.vetpro.co.uk/products/joints-and-mobility
**The Vet Corner groups encourage members to establish a relationship with their local veterinarian, don’t wait until an emergency.**
© 2014-2025 Rural Veterinary Outreach. All Rights Reserved.
You must be logged in to post a comment.